by Becca Renk, published on Casa Benjamin Linder, August 10, 2022
DENGUE FEVER
We’re settling in to our daughter Orla’s sixth night in the hospital. Visiting hours are over and only ten of the beds in our 32-bed pediatric ward are occupied tonight, down from 20 a few nights ago. The patients – mostly young teens in our room – are tucked in under mosquito nets. Their carers – mainly grandmas, aunts and moms – are slouched in chairs or curled around their patients on the beds. A few of us stretch out on unoccupied beds to get some rest before the nurse turns on the lights for the next regular blood pressure and temp check.
Our 14 year-old was admitted to the pediatric ward with dengue fever on July 19th, Revolution Day in Nicaragua. Poor Orla sobbed in disappointment that she wouldn’t be able to celebrate the holiday. After two days of fever, I had taken her to the emergency room in our local Ciudad Sandino Primary Hospital where the blood work they ordered indicated dengue and showed that her platelet count was low enough to be of concern. “She’ll be staying here with us,” the doctor announced. Since then, either my husband Paul or I have been with her in the hospital, tasked with making sure she’s kept hydrated and informed of her progress via blood test results each day.
Dengue fever is a virus transmitted by mosquitoes that propagate in the tropics during the rainy season and it affects 50 million people annually worldwide. Nicaragua works to control outbreaks through regular house-to-house fumigation and eliminating stagnant water – the epidemiology department of the health services visited our house shortly after Orla was hospitalized to get kill any mosquitoes or larvae. There is no cure for dengue, just symptom management over its eight-day cycle. The virus attacks the body and can cause leakage in vessel walls, resulting in water loss in the circulatory system and rapid dehydration. Much rarer severe cases can cause internal bleeding and for blood platelets to drop to dangerously low levels. Hemorrhagic dengue is particularly dangerous because patients can go into shock and die before they can get the blood transfusion they need.
Because of this risk, the Nicaraguan Ministry of Health’s policy is to hospitalize anyone with dengue who shows signs of possible complications, including low blood platelets. Thanks to this prudent policy and quality care, Nicaragua is the country with fewer deaths from dengue than any other country in the region – in a normal year, zero deaths. Treatment for the 12 pediatric patients we’ve seen come through our room has been intravenous rehydration fluids and ultrasounds upon being admitted; blood pressure, temp and blood oxygen level checks every two hours; daily blood tests; and constant monitoring of liquid intake and outflow. Patients with fevers get acetaminophen, patients with suspicious pain are taken for another ultrasound, patients not getting enough fluids are put back on IVs.
Although the staff has been concerned about possible complications for at least four of our patients, including Orla, no one on our ward has been transferred to a larger Managua hospital for emergency transfusions; but the ambulance is standing by outside if its needed. Knowing that gives me incredible peace of mind – at home, how could I possibly have known what Orla’s platelets were doing?
Growing up in the U.S., I never had a close family member admitted to the hospital; in fact, visits to the doctor were rare. As a kid, I remember knowing that if I got sick over the weekend, I’d have to tough it out until Monday when we could see the doctor during office hours. A trip to the emergency room at the hospital – the only after-hours option in my rural county – was too expensive. For the most part, everyone I knew only went to the doctor if they’d been sick for more than a week – their families simply couldn’t afford more frequent care.
By contrast, Nicaraguans seem to go to the doctor all the time. If my neighbor’s kid gets diarrhea, they bring her straight to the emergency room. I used to think this was because people were afraid – in the 1990s and early 2000s, child and infant mortality rates were high in Nicaragua and many kids really did die of preventable diseases. But as child health has improved – infant mortality down by 61% and chronic malnutrition reduced by 66% over the past 15 years – I have finally begun to understand that Nicaraguans take their kids to the hospital because they can.
Back in Idaho where I’m from, Orla’s emergency room visit alone would have cost $2,159 and her six nights in the hospital would have totaled more than $60,000. In the United States, medical debt cripples 41% of all U.S. adults and they scramble to pay outrageous bills: more than a quarter of all fundraisers on crowdfunding sites are for health-related costs.
My mom has been telling her friends in Idaho of our woes. “My granddaughter in Nicaragua has spent the week hospitalized with dengue fever.”
“Oh dear!” Her friends all exclaim (dengue fever does sound awfully dramatic).
“Guess how much their hospital bill is so far?” She asks. They frown and shake their heads, already anticipating that my mom is about to hit them up for donations for a GoFundMe campaign to help cover our bills.
“How much?” They ask.
“Nothing at all!” My mom gleefully reports. “Nicaragua has free universal health care!” Her friends’ shock is palpable. “How,” they ask, “can a poor country like Nicaragua afford to give free health care to its people?”
The answer, of course, is because Nicaragua chooses to make free health care a priority for its people.
NICARAGUA’S TRICKLE-UP ECONOMICS
Nighttime in the pediatric ward means little sleep for carers. In the morning I wake at three, holding a sleepy Orla upright while the lab tech gets a blood sample from her arm, and then try to coax a bit more fluid down her throat. Crash back into sleep until the nurse comes to collect the papers where we write down our patients’ intake and outflow and do the consequential math: are more fluids going in than coming out? Next the doctors arrive with the lab results for the day: who gets to go home and who has to stay. The hopeful have their bags packed, waiting. The feverish ones stay wrapped in restless sheets, in and out of consciousness, knowing they’ll be here another night.
On our third morning, I start awake at ten minutes to seven and rush to shower and change before my husband Paul arrives– bless him – with strong coffee and the car keys. I kiss Orla goodbye and drive straight from the hospital to interpret for a delegation that is in Nicaragua to celebrate the 43rd Anniversary of the Triumph of the Sandinista Revolution, when the Nicaraguan people overthrew the cruel Somoza dictatorship.
Our first meeting is with Nicaragua’s Finance Minister Iván Acosta. It’s my first time interpreting for him and I soon realize that even with a full-night’s sleep I couldn’t do him justice with my interpretation. He has an obvious grasp of details – quoting figures off the top of his head and speaking for two hours with no notes – but above all else, Minister Acosta is a Big Picture person. He connects the dots for us between policy, action and results, giving perspective to Nicaragua’s entire revolutionary project.
“When we came into office in 2007, following nearly 17 years of neoliberal governments,” he says, “we found the country in chaos.” Minister Acosta explains that the period from 1990 to 2006 when Nicaragua had followed structural adjustment policies of the World Bank and the International Monetary Fund led to extreme inequality, seriously deteriorated infrastructure, and deep poverty, particularly in Nicaragua’s countryside. “There was no magic solution for any of this. What could we do?” He asks.
Nicaragua’s Sandinista government decided on a blend of social responsibility and economic principles. They began restoring rights – to free health care, free public education and land tenure. But they also worked to find ways to ensure that Nicaragua’s poor majority became active participants in the economy as a solution to improve the country’s struggling economy. “We realized that we need to lower the cost of doing business to be competitive; in order to achieve that, we needed to increase public spending.”
To that end, Nicaragua set about building state-of-the-art roads – now the best in the region – to ensure that products could get to market cheaply and easily; improving access to basic services – now reaching 99% electrical coverage up from just 53% in 2006; ending 12-hour a day rolling blackouts and diversifying to generate clean energy – now 80% of the electricity produced is from renewables; training new teachers and building new schools; and building 24 new hospitals since 2007. Over just ten years, Minister Acosta explains, social spending went from being 10% of overall spending to making up 57% of the country’s budget. But have these policies been effective?
“We have these pro-poor policies, but in many countries only lip service is paid to political policy and it isn’t followed by action,” explains Minister Acosta. “So we do the math – all the various quotients and formulae recommended by international experts – to ensure that our policies are being translated into results: real improvements in the lives of the poor.”
The numbers show that not only has Nicaragua’s economy turned around – sustained GDP growth of 5-10%, historic international investment, and 90% food sovereignty have all been achieved – but also the lives of the country’s poor majority have improved. In 2006, GDP per capita was at $990, but by 2018 it had risen to $2,300. “We don’t have a significant middle class yet,” Minister Acosta cautions, but progress is being made.
Nicaragua’s policy could be described as “trickle up economics” – ensure the poor access to health care, education, land, markets, financing…and the economy will follow.
This is the inversion of “trickle down economics,” the U.S. policy made famous by Ronald Reagan which gives tax breaks and benefits to corporations and the wealthy on the theory that it will stimulate economic growth from the top down.
The problem with the U.S. policy is not only a moral one; in economic terms, it just plain doesn’t work.
Under four decades of “trickle down” policy, income inequality in the U.S. has grown to shocking levels: the wealthiest 0.1% have become rich beyond all comprehension, while most U.S. workers now earn less than half of what they would have been earning if incomes had continued to grow equitably.
In other words, tax breaks and benefits to the richest simply don’t trickle down: US families now work longer hours for less pay while struggling to cover skyrocketing costs. Currently, 22% of the U.S. population can’t access health care due to lack of adequate insurance, 12% experiences hunger and more than half a million people are homeless –many living under the country’s collapsing bridges – one in every five of which are in need of reconstruction.
Given what we know about how stability and quality of life for the majority can improve the overall economy, perhaps instead of asking “How can a poor country like Nicaragua afford to give free health care to its people?” We should really be asking, “How can a wealthy country like the United States afford NOT to?”
NICARAGUA’S COMMUNITY AND FAMILY-BASED HEALTH MODEL
“Dengue is treacherous,” the doctor explains to me. “A patient can suddenly experience internal bleeding and become critical in the blink of an eye.” Orla’s platelets have dropped, and she is in the most crucial day in the virus’ cycle when signs of hemorrhagic dengue can appear. As I sit on the edge of her bed urging her to drink more rehydration fluid, a woman who has been visiting another patient comes over to Orla’s bed carrying a Bible.
“Would you like me to pray for your daughter?” She asks. Orla agrees and the woman asks, “Have you accepted Jesus Christ as your Lord and Savior?” I stop her, not wanting her to get the wrong idea. “We’re not Pentecostals,” I say, “but Orla believes in God.” The woman nods and holds her hands out, palms up. We close our eyes as she begins praying in a soft singsong voice, asking God to look after my baby and heal her. When she finishes, she surprises me by saying, “It doesn’t matter which religion we belong to, it’s all the same God.”
That day, Orla turns a corner – her fever drops and her health begins to improve. I’m grateful to all those responsible – as we say here in Nicaragua, “Thanks to God and the Revolution.” Why the Revolution? Because it has restored Nicaraguans’ rights to free quality health care.
Our entire delegation gets to see the quality of this health care up close. After our talk with Minister Acosta, we visit one of the best-equipped hospitals in the country, Velez Paíz, built new and opened in 2018. Director Dr. Virginia Garcia tells us that patients with non-urgent emergencies wait a maximum of 30 minutes to be seen by ER doctors, and that patients wait a maximum of one month for non-emergency surgeries. “We have four laparoscopic towers performing gall bladder surgeries all day every day,” she says; that surgery would cost $54,000 in my home country, but is free in Nicaragua.
I interpret for Minister of Health Dr. Martha Reyes when she describes to the delegation the advances made in public health over the past 15 years. As she speaks, it is easy for me to chart that path from policy to action to results that Minister Acosta talked about. When she finishes speaking, I thank Dr. Reyes personally for the quality care that Orla is receiving in our hometown public hospital. “Not so long ago,” I tell her, “that wouldn’t have been possible.”
When I moved to Ciudad Sandino twenty years ago, our hospital was literally an empty shell, unable to provide even the most basic services to our community of 180,000. Not only did patients in “public” hospitals have to pay for everything from gloves to sutures, but a dengue patient in Orla’s condition would have actually been safer at home – hospitals were in such appalling conditions with lack of staff, beds and even basic sanitation that it was commonly said that hospitals were where patients went to die.
Thanks to public investment in health infrastructure, increase in personnel, improved and specialized training, and tireless work to involve communities and families in their own health care, Ciudad Sandino now has seven health centers and a hospital which includes outpatient, inpatient and emergency care, a maternal wait home, rehabilitation and physical therapy services, a natural medicine center and a center for cataract surgeries – all services offered free of charge. Comparable improvements have happened all over the country – the change in people’s lives is palpable and the results in overall health are measureable: maternal mortality rates have dropped by 70%, deaths from cervical cancer are down by 25% and average life expectancy has increased.
THE PRIVILEGE OF FREE HEALTH CARE
On the morning of Orla’s seventh day in the hospital, the doctor tells us that her platelets count is high enough to safely send her home. We leave the hospital with nothing more than her official diagnosis paper, a stamped doctor’s excuse for missing school, and a follow up appointment. We owe no money. There is no itemized bill showing how many nights (6), how many sheets were washed (3), how many cafeteria meals she ate (17), how many full blood tests (10), urine tests (1), ultrasounds (1), IVs (1), or how much oral rehydration fluid she drank (53 liters). Orla and I walk out into the sunshine of a new day, ready to rest and recover, secure in the knowledge that the Nicaraguan government has made a choice to look after us…recognizing that it is a privilege to have access to free quality health care.
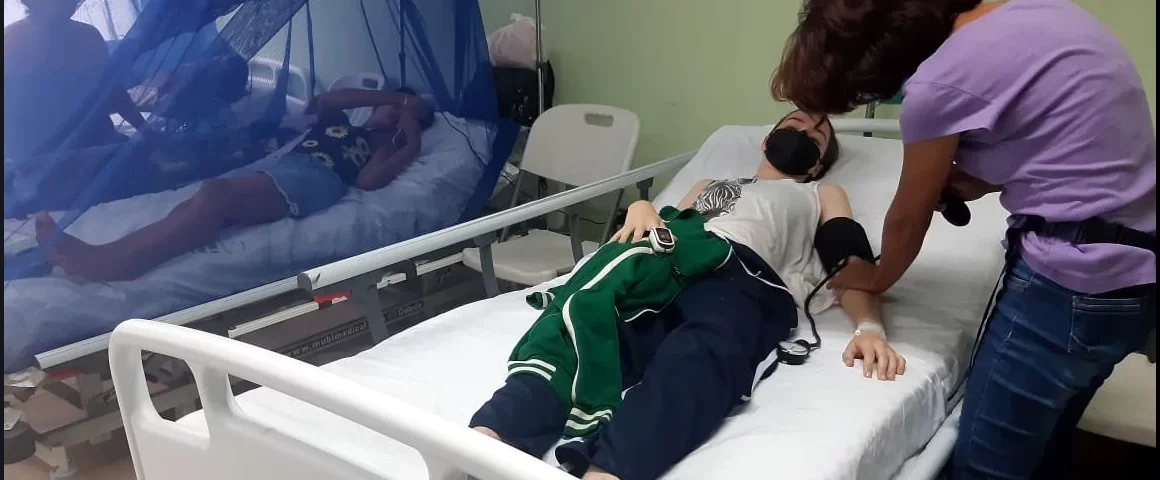
*Featured Image: Orla getting blood pressure checked in the hospital.
Becca Renk has lived and worked in sustainable community development in Nicaragua since 2001 with the Jubilee House Community and its project, the Center for Development in Central America. The JHC-CDCA also works to educate visitors to Nicaragua, including through their hospitality and solidarity cultural center at Casa Benjamin Linder.